The Myth of Drug Expiration Dates
by Marshall Allen, ProPublica
Hospitals and pharmacies are required to toss expired drugs, no matter how expensive or vital. Meanwhile the FDA has long known that many remain safe and potent for years longer.
This story was co-published with NPR’s Shots blog.
The box of prescription drugs had been forgotten in a back closet of a retail pharmacy for so long that some of the pills predated the 1969 moon landing. Most were 30 to 40 years past their expiration dates — possibly toxic, probably worthless.
But to Lee Cantrell, who helps run the California Poison Control System, the cache was an opportunity to answer an enduring question about the actual shelf life of drugs: Could these drugs from the bell-bottom era still be potent?
Cantrell called Roy Gerona, a University of California, San Francisco, researcher who specializes in analyzing chemicals. Gerona had grown up in the Philippines and had seen people recover from sickness by taking expired drugs with no apparent ill effects.
“This was very cool,” Gerona says. “Who gets the chance of analyzing drugs that have been in storage for more than 30 years?”
The age of the drugs might have been bizarre, but the question the researchers wanted to answer wasn’t. Pharmacies across the country — in major medical centers and in neighborhood strip malls — routinely toss out tons of scarce and potentially valuable prescription drugs when they hit their expiration dates.
Gerona and Cantrell, a pharmacist and toxicologist, knew that the term “expiration date” was a misnomer. The dates on drug labels are simply the point up to which the Food and Drug Administration and pharmaceutical companies guarantee their effectiveness, typically at two or three years. But the dates don’t necessarily mean they’re ineffective immediately after they “expire” — just that there’s no incentive for drugmakers to study whether they could still be usable.
ProPublica has been researching why the U.S. health care system is the most expensive in the world. One answer, broadly, is waste — some of it buried in practices that the medical establishment and the rest of us take for granted. We’ve documented how hospitals often discard pricey new supplies, how nursing homes trash valuable medications after patients pass away or move out, and how drug companies create expensive combinations of cheap drugs. Experts estimate such squandering eats up about $765 billion a year — as much as a quarter of all the country’s health care spending.
Help Us Investigate Wasted Health Care Dollars
Experts say the United States might be squandering a quarter of the money spent on health care. That’s an estimated $765 billion a year. Do you believe you’ve encountered this waste? Tell us.
What if the system is destroying drugs that are technically “expired” but could still be safely used?
In his lab, Gerona ran tests on the decades-old drugs, including some now defunct brands such as the diet pills Obocell (once pitched to doctors with a portly figurine called “Mr. Obocell”) and Bamadex. Overall, the bottles contained 14 different compounds, including antihistamines, pain relievers and stimulants. All the drugs tested were in their original sealed containers.
The findings surprised both researchers: A dozen of the 14 compounds were still as potent as they were when they were manufactured, some at almost 100 percent of their labeled concentrations.
“Lo and behold,” Cantrell says, “The active ingredients are pretty darn stable.”
Cantrell and Gerona knew their findings had big implications. Perhaps no area of health care has provoked as much anger in recent years as prescription drugs. The news media is rife with stories of medications priced out of reach or of shortages of crucial drugs, sometimes because producing them is no longer profitable.
Tossing such drugs when they expire is doubly hard. One pharmacist at Newton-Wellesley Hospital outside Boston says the 240-bed facility is able to return some expired drugs for credit, but had to destroy about $200,000 worth last year. A commentary in the journal Mayo Clinic Proceedings cited similar losses at the nearby Tufts Medical Center. Play that out at hospitals across the country and the tab is significant: about $800 million per year. And that doesn’t include the costs of expired drugs at long-term care pharmacies, retail pharmacies and in consumer medicine cabinets.
After Cantrell and Gerona published their findings in Archives of Internal Medicine in 2012, some readers accused them of being irresponsible and advising patients that it was OK to take expired drugs. Cantrell says they weren’t recommending the use of expired medication, just reviewing the arbitrary way the dates are set.
“Refining our prescription drug dating process could save billions,” he says.
But after a brief burst of attention, the response to their study faded. That raises an even bigger question: If some drugs remain effective well beyond the date on their labels, why hasn’t there been a push to extend their expiration dates?
It turns out that the FDA, the agency that helps set the dates, has long known the shelf life of some drugs can be extended, sometimes by years.
In fact, the federal government has saved a fortune by doing this.
For decades, the federal government has stockpiled massive stashes of medication, antidotes and vaccines in secure locations throughout the country. The drugs are worth tens of billions of dollars and would provide a first line of defense in case of a large-scale emergency.
Maintaining these stockpiles is expensive. The drugs have to be kept secure and at the proper humidity and temperature so they don’t degrade. Luckily, the country has rarely needed to tap into many of the drugs, but this means they often reach their expiration dates. Though the government requires pharmacies to throw away expired drugs, it doesn’t always follow these instructions itself. Instead, for more than 30 years, it has pulled some medicines and tested their quality.
The idea that drugs expire on specified dates goes back at least a half-century, when the FDA began requiring manufacturers to add this information to the label. The time limits allow the agency to ensure medications work safely and effectively for patients. To determine a new drug’s shelf life, its maker zaps it with intense heat and soaks it with moisture to see how it degrades under stress. It also checks how it breaks down over time. The drug company then proposes an expiration date to the FDA, which reviews the data to ensure it supports the date and approves it. Despite the difference in drugs’ makeup, most “expire” after two or three years.
Pharmacists and researchers say there is no economic “win” for drug companies to investigate further. They ring up more sales when medications are tossed as “expired” by hospitals, retail pharmacies and consumers despite retaining their safety and effectiveness.
Industry officials say patient safety is their highest priority. Olivia Shopshear, director of science and regulatory advocacy for the drug industry trade group Pharmaceutical Research and Manufacturers of America, or PhRMA, says expiration dates are chosen “based on the period of time when any given lot will maintain its identity, potency and purity, which translates into safety for the patient.”
That being said, it’s an open secret among medical professionals that many drugs maintain their ability to combat ailments well after their labels say they don’t. One pharmacist says he sometimes takes home expired over-the-counter medicine from his pharmacy so he and his family can use it.
The federal agencies that stockpile drugs — including the military, the Centers for Disease Control and Prevention and the Department of Veterans Affairs — have long realized the savings in revisiting expiration dates.
In 1986, the Air Force, hoping to save on replacement costs, asked the FDA if certain drugs’ expiration dates could be extended. In response, the FDA and Defense Department created the Shelf Life Extension Program.
Each year, drugs from the stockpiles are selected based on their value and pending expiration and analyzed in batches to determine whether their end dates could be safely extended. For several decades, the program has found that the actual shelf life of many drugs is well beyond the original expiration dates.
A 2006 study of 122 drugs tested by the program showed that two-thirds of the expired medications were stable every time a lot was tested. Each of them had their expiration dates extended, on average, by more than four years, according to research published in the Journal of Pharmaceutical Sciences.
Some that failed to hold their potency include the common asthma inhalant albuterol, the topical rash spray diphenhydramine, and a local anesthetic made from lidocaine and epinephrine, the study said. But neither Cantrell nor Dr. Cathleen Clancy, associate medical director of National Capital Poison Center, a nonprofit organization affiliated with the George Washington University Medical Center, had heard of anyone being harmed by any expired drugs. Cantrell says there has been no recorded instance of such harm in medical literature.
Marc Young, a pharmacist who helped run the extension program from 2006 to 2009, says it has had a “ridiculous” return on investment. Each year the federal government saved $600 million to $800 million because it did not have to replace expired medication, he says.
An official with the Department of Defense, which maintains about $13.6 billion worth of drugs in its stockpile, says that in 2016 it cost $3.1 million to run the extension program, but it saved the department from replacing $2.1 billion in expired drugs. To put the magnitude of that return on investment into everyday terms: It’s like spending a dollar to save $677.
“We didn’t have any idea that some of the products would be so damn stable — so robustly stable beyond the shelf life,” says Ajaz Hussain, one of the scientists who formerly helped oversee the extension program.
Hussain is now president of the National Institute for Pharmaceutical Technology and Education, an organization of 17 universities that’s working to reduce the cost of pharmaceutical development. He says the high price of drugs and shortages make it time to reexamine drug expiration dates in the commercial market.
“It’s a shame to throw away good drugs,” Hussain says.
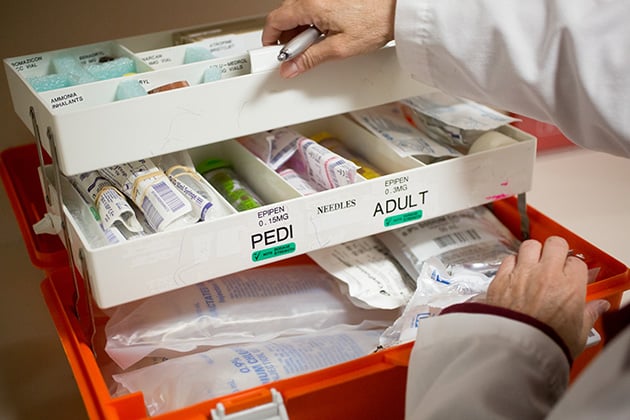
The drugs kept in emergency crash carts at Newton-Wellesley Hospital, outside Boston, Massachusetts, often expire before they can be used and must be thrown away. (Erik Jacobs for ProPublica)
Some medical providers have pushed for a changed approach to drug expiration dates — with no success. In 2000, the American Medical Association, foretelling the current prescription drug crisis, adopted a resolution urging action. The shelf life of many drugs, it wrote, seems to be “considerably longer” than their expiration dates, leading to “unnecessary waste, higher pharmaceutical costs, and possibly reduced access to necessary drugs for some patients.”
Citing the federal government’s extension program, the AMA sent letters to the FDA, the U.S. Pharmacopeial Convention, which sets standards for drugs, and PhRMA asking for a re-examination of expiration dates.
No one remembers the details — just that the effort fell flat.
“Nothing happened, but we tried,” says rheumatologist Roy Altman, now 80, who helped write the AMA report. “I’m glad the subject is being brought up again. I think there’s considerable waste.”
At Newton-Wellesley Hospital, outside Boston, pharmacist David Berkowitz yearns for something to change.
On a recent weekday, Berkowitz sorted through bins and boxes of medication in a back hallway of the hospital’s pharmacy, peering at expiration dates. As the pharmacy’s assistant director, he carefully manages how the facility orders and dispenses drugs to patients. Running a pharmacy is like working in a restaurant because everything is perishable, he says, “but without the free food.”
Federal and state laws prohibit pharmacists from dispensing expired drugs and The Joint Commission, which accredits thousands of health care organizations, requires facilities to remove expired medication from their supply. So at Newton-Wellesley, outdated drugs are shunted to shelves in the back of the pharmacy and marked with a sign that says: “Do Not Dispense.” The piles grow for weeks until they are hauled away by a third-party company that has them destroyed. And then the bins fill again.
“I question the expiration dates on most of these drugs,” Berkowitz says.
One of the plastic boxes is piled with EpiPens — devices that automatically inject epinephrine to treat severe allergic reactions. They run almost $300 each. These are from emergency kits that are rarely used, which means they often expire. Berkowitz counts them, tossing each one with a clatter into a separate container, “… that’s 45, 46, 47 …” He finishes at 50. That’s almost $15,000 in wasted EpiPens alone.

In May, Cantrell and Gerona published a study that examined 40 EpiPens and EpiPen Jrs., a smaller version, that had been expired for between one and 50 months. The devices had been donated by consumers, which meant they could have been stored in conditions that would cause them to break down, like a car’s glove box or a steamy bathroom. The EpiPens also contain liquid medicine, which tends to be less stable than solid medications.
Testing showed 24 of the 40 expired devices contained at least 90 percent of their stated amount of epinephrine, enough to be considered as potent as when they were made. All of them contained at least 80 percent of their labeled concentration of medication. The takeaway? Even EpiPens stored in less than ideal conditions may last longer than their labels say they do, and if there’s no other option, an expired EpiPen may be better than nothing, Cantrell says.
At Newton-Wellesley, Berkowitz keeps a spreadsheet of every outdated drug he throws away. The pharmacy sends what it can back for credit, but it doesn’t come close to replacing what the hospital paid.
Then there’s the added angst of tossing drugs that are in short supply. Berkowitz picks up a box of sodium bicarbonate, which is crucial for heart surgery and to treat certain overdoses. It’s being rationed because there’s so little available. He holds up a purple box of atropine, which gives patients a boost when they have low heart rates. It’s also in short supply. In the federal government’s stockpile, the expiration dates of both drugs have been extended, but they have to be thrown away by Berkowitz and other hospital pharmacists.
The 2006 FDA study of the extension program also said it pushed back the expiration date on lots of mannitol, a diuretic, for an average of five years. Berkowitz has to toss his out. Expired naloxone? The drug reverses narcotic overdoses in an emergency and is currently in wide use in the opioid epidemic. The FDA extended its use-by date for the stockpiled drugs, but Berkowitz has to trash it.
On rare occasions, a pharmaceutical company will extend the expiration dates of its own products because of shortages. That’s what happened in June, when the FDA posted extended expiration dates from Pfizer for batches of its injectable atropine, dextrose, epinephrine and sodium bicarbonate. The agency notice included the lot numbers of the batches being extended and added six months to a year to their expiration dates.

David Berkowitz, assistant director of the pharmacy at Newton-Wellesley Hospital, said he questions the validity of many drug expiration dates. (Erik Jacobs for ProPublica)
Berkowitz says he appreciated Pfizer’s action, but feels it should be standard to make sure drugs that are still effective aren’t thrown away.
“The question is: Should the FDA be doing more stability testing?” Berkowitz says. “Could they come up with a safe and systematic way to cut down on the drugs being wasted in hospitals?”
Four scientists who worked on the FDA extension program told ProPublica something like that could work for drugs stored in hospital pharmacies, where conditions are carefully controlled.
Greg Burel, director of the CDC’s stockpile, says he worries that if drugmakers were forced to extend their expiration dates it could backfire, making it unprofitable to produce certain drugs and thereby reducing access or increasing prices.
The 2015 commentary in Mayo Clinic Proceedings, called “Extending Shelf Life Just Makes Sense,” also suggested that drugmakers could be required to set a preliminary expiration date and then update it after long-term testing. An independent organization could also do testing similar to that done by the FDA extension program, or data from the extension program could be applied to properly stored medications.
ProPublica asked the FDA whether it could expand its extension program, or something like it, to hospital pharmacies, where drugs are stored in stable conditions similar to the national stockpile.
“The Agency does not have a position on the concept you have proposed,” an official wrote back in an email.
Whatever the solution, the drug industry will need to be spurred in order to change, says Hussain, the former FDA scientist. “The FDA will have to take the lead for a solution to emerge,” he says. “We are throwing away products that are certainly stable, and we need to do something about it.”
After I was prescribed a brand-name drug I didn’t need and given a coupon to cover the out-of-pocket costs, I discovered another reason Americans pay too much for health care.
 Wasted Medicine Billions of dollars are routinely wasted every day by health care providers in the United States — and it’s driving up the cost of care for all of us.
Wasted Medicine Billions of dollars are routinely wasted every day by health care providers in the United States — and it’s driving up the cost of care for all of us.
This story was co-published with The Atlantic.
Everything happened so fast as I walked out of the doctor’s exam room. I was tucking in my shirt and wondering if I’d asked all my questions about my injured shoulder when one of the doctor’s assistants handed me two small boxes of pills.
“These will hold you over until your prescription arrives in the mail,” she said, pointing to the drug samples.
Strange, I thought to myself, the doctor didn’t mention giving me any drugs.
I must have looked puzzled because she tried to reassure me.
“Don’t worry,” she said. “It won’t cost you any more than $10.”
I was glad whatever was coming wouldn’t break my budget, but I didn’t understand why I needed the drugs in the first place. And why wasn’t I picking them up at my local CVS?
At first I shrugged it off. This had been my first visit with an orthopedic specialist and he, Dr. Mohnish Ramani, hadn’t been the chatty type. He’d barely said a word as he examined me, tugging my arm this way and bending it that way before rotating it behind my back. The pain made me squirm and yelp, but he knew what he was doing. He promptly diagnosed me with frozen shoulder, a debilitating inflammation of the shoulder capsule.
But back to the drugs. As an investigative reporter who has covered health care for more than a decade, the interaction was just the sort of thing to pique my interest. One thing I’ve learned is that almost nothing in medicine — especially brand-name drugs — is ever really a deal. When I got home, I looked up the drug: Vimovo.
The drug has been controversial, to say the least. Vimovo was created using two readily and cheaply available generic, or over-the-counter, medicines: naproxen, also known by the brand Aleve, and esomeprazole magnesium, also known as Nexium. The Aleve handles your pain and the Nexium helps with the upset stomach that’s sometimes caused by the pain reliever. The key selling point of this new “convenience drug”? It’s easier to take one pill than two.
Experts say the United States might be squandering a quarter of the money spent on health care. That’s an estimated $765 billion a year. Do you believe you’ve encountered this waste? Tell us.
But only a minority of patients get an upset stomach, and there was no indication I’d be one of them. Did I even need the Nexium component?
Of course I also did the math. You can walk into your local drugstore and buy a month’s supply of Aleve and Nexium for about $40. For Vimovo, the pharmacy billed my insurance company $3,252. This doesn’t mean the drug company ultimately gets paid that much. The pharmaceutical world is rife with rebates and side deals — all designed to elbow ahead of the competition. But apparently the price of convenience comes at a steep mark-up.
Think about it another way. Let’s say you want to eat a peanut butter and jelly sandwich every day for a month. You could buy a big jar of peanut butter and a jar of grape jelly for less than 10 bucks. Or you could buy some of that stuff where they combine the peanut butter and grape jelly into the same jar. Smucker’s makes it. It’s called Goober. Except in this scenario, instead of its usual $3.50 price tag, Smucker’s is charging $565 for the jar of Goober.
So if Vimovo is the Goober of drugs, then why have Americans been spending so much on it? My insurance company, smartly, rejected the pharmacy’s claim. But I knew Vimovo’s makers weren’t wooing doctors like mine for nothing. So I looked up the annual reports for the Ireland-based company, Horizon Pharma, which makes Vimovo. Since 2014, Vimovo’s net sales have been more than $455 million. That means a lot of insurers are paying way more than they should for their Goober.
And Vimovo wasn’t Horizon’s only such drug. It has brought in an additional $465 million in net sales from Duexis, a similar convenience drug that combines ibuprofen and famotidine, AKA Advil and Pepcid.
This year I have been documenting the kind of waste in the health care system that’s not typically tracked. Americans pay more for health care than anyone else in the world, and experts estimate that the U.S. system wastes hundreds of billions of dollars a year. In recent months I’ve looked at what hospitals throw away and how nursing homes flush or toss out hundreds of millions of dollars’ worth of usable medicine every year. We all pay for this waste, through lower wages and higher premiums, deductibles and out-of-pocket costs. There doesn’t seem to be an end in sight — I just got a notice that my premiums may be increasing by another 12 percent next year.
With Vimovo, it seemed I stumbled on another waste stream: overpriced drugs whose actual costs are hidden from doctors and patients. In the case of Horizon, the brazenness of its approach was even more astounding because it had previously been called out in media reports and in a 2016 congressional hearing on out-of-control drug prices.
Health care economists also were wise to it.
“It’s a scam,” said Devon Herrick, a health care economist with the National Center for Policy Analysis. “It is just a way to gouge insurance companies or employer health care plans.”
Unsurprisingly, Horizon says the high price is justified. In fact, the drug maker wrote in an email, “The price of Vimovo is based on the value it brings to patients.” (sic)
Thousands of patients die and suffer injuries every year, the company said, because of gastric complications from naproxen and other non-steroid anti-inflammatory drugs (NSAIDs). Providing pain relief and stomach protection in a single pill makes it more likely patients will be protected from complications, it said.
And Horizon stressed Vimovo is a “special formulation” of Aleve and Nexium, so it’s not the same as taking the two separately. But several experts said that’s a scientific distinction that doesn’t make a therapeutic difference. “I would take the two medications from the drugstore in a heartbeat — therapeutically it makes sense,” said Michael Fossler, a pharmacist and clinical pharmacologist who is chair of the public-policy committee for the American College of Clinical Pharmacology. “What you’re paying for with [Vimovo] is the convenience. But it does seem awful pricey for that.”
Public outrage is boiling over when it comes to high drug prices, leading the media and lawmakers to scold pharmaceutical companies. You’d think a regulator would monitor this, but the Food and Drug Administration told me they are only authorized to review new drugs for safety and effectiveness, not prices. “Prices are set by manufacturers and distributors,” the FDA said in a statement.
Horizon acquired Vimovo in November 2013 from the global pharmaceutical giant AstraZeneca. Horizon knew it faced challenges trying to get top dollar for inexpensive ingredients. “Use of these therapies separately in generic form may be cheaper,” it said in its 2013 report to investors. But the company executed a shrewd strategy to give everyone — insurers, patients, doctors and pharmacies — the incentive to use Vimovo. It’s instructive to review its playbook.
To get Vimovo covered, Horizon made deals with insurance payers and pharmacy benefit managers — the intermediaries who help determine which drugs get reimbursed. The contracts generally included special rebates and even administrative fees for these intermediaries, the Horizon reports said, so the drug maker got paid much less than the sticker price, though it wouldn’t say how much. But the company’s net sales show the deals worked.
Horizon put boots on the ground to get the prescriptions rolling, expanding its sales force by the hundreds and focusing its marketing and sales efforts on doctors who already liked to prescribe brand-name drugs. The company’s message to doctors emphasized the convenience of prescribing the two ingredients in a single pill and that the single pill protected patients by making it more likely they would take their medication as directed.
Horizon also primed the medical community by giving donations totaling $101,000 to the American Gastroenterology Association, a specialty nonprofit for physicians. Some doctors refuse drug-industry money, if only to at least avoid the appearance of a conflict of interest. ProPublica has done loads of stories showing why doctors taking money is indeed problematic, including one about drug makers’ influence on physician specialty groups. When I went on the American Gastroenterology Association’s website, the first thing I saw was a pop-up ad from a drug company. Several of the association’s board members have received drug-company money, too. Horizon has made clear in its annual reports that donations to the group “help physicians and patients better understand and manage” the risks of pain relievers causing gastric problems.
Horizon also zeroed in on patients’ worries about drug costs. To encourage them to fill their prescriptions, Horizon covered all or most of their out-of-pocket costs. That’s why my doctor’s office could promise me I wouldn’t spend too much for my Vimovo. The program, Horizon told investors in reports, addressed the impact of pharmacies switching to less expensive alternatives and could “mitigate” the effect of payers searching for cheaper alternatives. (An infernal system, indeed.—Editors.)
The strategy worked on me. I didn’t even know why I was getting the prescription, but when they told me it wouldn’t cost more than I would spend on lunch with a friend, I gave it the OK. A pharmacy I’d never heard of sent me a bottle of Vimovo for $10, even though my insurance company rejected the claim.
Turns out paying the patient’s costs motivated my doctor, too. I waited until the end of my next visit to bring up Vimovo, and then we had a follow-up conversation on the phone. Ramani didn’t know the price of the drug and found it “disturbing” when I told him. That was a surprise to me, but not to him. He said he leaves billing to his staff and doesn’t even know how much he gets paid for a lot of the procedures he performs, let alone how much insurers are being charged for drugs. The marketing arms of companies like Horizon must count on this sort of blindness.
Ramani doesn’t receive money or gifts from Horizon. (I confirmed this on ProPublica’s Dollars for Docs website, which lists drug-company payments.) He said he likes Vimovo because Horizon covers the patient’s out-of-pocket costs, entirely in many cases. Prescribing the generics or over-the-counter medications separately would actually cost more, he said. Which of course is exactly the company’s plan. But Ramani agreed that the high cost of the drug to insurers ultimately raises overall health care costs for all Americans.
Knowing Vimovo’s price, I asked him if he would continue to prescribe it. “It changes my thought process,” he said. “But at the end of the day, I have to think about the patient and whether the patient will be able to pay out of pocket or not.”
Ramani said the Horizon drug rep told him Vimovo prescriptions had to go through a particular pharmacy for the patient to receive financial assistance. In its 2016 annual report, Horizon wrote that prescriptions for its drugs might not be filled by certain pharmacies because of insurance-company exclusions, co-payment requirements, or incentives to use lower-priced alternatives. So that’s why they didn’t give me the option of picking up my pills at my neighborhood drugstore.
Instead, my Vimovo was mailed to me from White Oak Pharmacy in Nutley, New Jersey, which is about 45 minutes from my house. I drove there to find out why. The neighborhood pharmacy is on the bottom floor of a two-story brick building on a street corner, next to a hair salon.
Vishal Chhabria, the pharmacist who owns White Oak, told me the drug company sets the price of Vimovo. He insisted his pharmacy has no special relationship or contract with Horizon. Maybe the drug company steers prescriptions his way, he said, because his pharmacy will process the coupons that reduce or eliminate the patient costs, which some pharmacies don’t.
Chhabria said there is no approved generic alternative to Vimovo, so he can’t suggest one to patients. And while other drugs, like over-the-counter medications, would be cheaper for the health system overall, they are more expensive for the individual patient, he said.
In poring through Horizon’s financial filings, it appears the drug’s run may be ending. Horizon said in its report for the first quarter of 2017 that fewer insurance companies have been willing to cover Vimovo and many that do have demanded larger rebates. As a result, Horizon has been eating more of the costs of providing the drug to patients, as they must have in my case. The prescriptions have still been coming in, but net sales were just under $5 million in the first quarter of this year, down 81 percent from the first quarter of 2016.
Critics of Vimovo say that’s still more than patients should be spending on the drug. “That number should be zero,” said Linda Cahn, an attorney who advises corporations, unions and other payers to help reduce their costs. “If you want to talk about waste, that’s waste.”
Herrick, the health care economist, said Horizon cashed in by eliminating many of the barriers in the system that are meant to control costs. The company got patients on board by covering their out-of-pocket costs. It appealed to doctors by promoting the benefits to patients. And it did an end-run around chain pharmacies, which typically might suggest a lower-priced alternative, by steering prescriptions to pharmacists who would participate in their patient-assistance program.
“Somebody brainstormed: ‘How can we nullify any consumer check and balance in this supply chain? What can we do to keep the customer from asking questions?’” Herrick said.
The scheme that played out with Vimovo is bound to happen again, Herrick said. Maybe it already is. Drug companies are always on the lookout to deploy similar strategies.
I dutifully took my Vimovo for several days, until I noticed it kept me awake until 3 in the morning — a rare side effect. (Perhaps they need to add a third drug to the combo.) I probably have more than 50 pills left in the bottle on my bedside table. Maybe I could sell it back to Horizon for $1,500.
 Marshall Allen covers patient safety for ProPublica. He is one of the creators of ProPublica’s Surgeon Scorecard, which published the complication rates for about 17,000 surgeons who perform eight common elective procedures. He also moderates the ProPublica Patient Safety Facebook group. Allen’s work has been honored with several journalism awards, including the Harvard Kennedy School’s 2011 Goldsmith Prize for Investigative Reporting and coming in as a finalist for the Pulitzer Prize for local reporting for work at the Las Vegas Sun, where he worked before coming to ProPublica in 2011. Before he was in journalism, Allen spent five years in full-time ministry, including three years in Nairobi, Kenya. He has a Master’s degree in Theology.
Marshall Allen covers patient safety for ProPublica. He is one of the creators of ProPublica’s Surgeon Scorecard, which published the complication rates for about 17,000 surgeons who perform eight common elective procedures. He also moderates the ProPublica Patient Safety Facebook group. Allen’s work has been honored with several journalism awards, including the Harvard Kennedy School’s 2011 Goldsmith Prize for Investigative Reporting and coming in as a finalist for the Pulitzer Prize for local reporting for work at the Las Vegas Sun, where he worked before coming to ProPublica in 2011. Before he was in journalism, Allen spent five years in full-time ministry, including three years in Nairobi, Kenya. He has a Master’s degree in Theology.
In May, Cantrell and Gerona published a study that examined 40 EpiPens and EpiPen Jrs., a smaller version, that had been expired for between one and 50 months. The devices had been donated by consumers, which meant they could have been stored in conditions that would cause them to break down, like a car’s glove box or a steamy bathroom. The EpiPens also contain liquid medicine, which tends to be less stable than solid medications.
[premium_newsticker id=”154171″]
Parting shot—a word from the editors
The Best Definition of Donald Trump We Have Found
 In his zeal to prove to his antagonists in the War Party that he is as bloodthirsty as their champion, Hillary Clinton, and more manly than Barack Obama, Trump seems to have gone “play-crazy” -- acting like an unpredictable maniac in order to terrorize the Russians into forcing some kind of dramatic concessions from their Syrian allies, or risk Armageddon.However, the “play-crazy” gambit can only work when the leader is, in real life, a disciplined and intelligent actor, who knows precisely what actual boundaries must not be crossed. That ain’t Donald Trump -- a pitifully shallow and ill-disciplined man, emotionally handicapped by obscene privilege and cognitively crippled by white American chauvinism. By pushing Trump into a corner and demanding that he display his most bellicose self, or be ceaselessly mocked as a “puppet” and minion of Russia, a lesser power, the War Party and its media and clandestine services have created a perfect storm of mayhem that may consume us all.— Glen Ford, Editor in Chief, Black Agenda Report
In his zeal to prove to his antagonists in the War Party that he is as bloodthirsty as their champion, Hillary Clinton, and more manly than Barack Obama, Trump seems to have gone “play-crazy” -- acting like an unpredictable maniac in order to terrorize the Russians into forcing some kind of dramatic concessions from their Syrian allies, or risk Armageddon.However, the “play-crazy” gambit can only work when the leader is, in real life, a disciplined and intelligent actor, who knows precisely what actual boundaries must not be crossed. That ain’t Donald Trump -- a pitifully shallow and ill-disciplined man, emotionally handicapped by obscene privilege and cognitively crippled by white American chauvinism. By pushing Trump into a corner and demanding that he display his most bellicose self, or be ceaselessly mocked as a “puppet” and minion of Russia, a lesser power, the War Party and its media and clandestine services have created a perfect storm of mayhem that may consume us all.— Glen Ford, Editor in Chief, Black Agenda Report